INTRODUCTION
Gastrointestinal (GI) disturbances, including acute gastritis, are common in dogs and can manifest with a variety of clinical signs, such as vomiting, diarrhea, and abdominal pain [1, 2]. One of the challenges veterinarians face in diagnosing the exact cause of such disturbances is the limited range of available noninvasive diagnostic tools. Traditional diagnostic modalities, such as radiography or ultrasound provide limited insights into mucosal surfaces and may not always effectively pinpoint the cause of the disturbance [1, 2].
Endoscopy is the gold standard for visual examination of the internal lining of the GI tract, facilitating the identification of inflammation, ulcers, and other pathologies [3, 4]. However, the procedure typically requires general anesthesia, which may pose risks for certain patients, especially those with underlying health conditions such as heart diseases.
Capsule endoscopy, a relatively recent advancement in veterinary medicine, offers a noninvasive approach for visualizing the entire GI tract without the need for anesthesia [5–9]. Given the minimal risk and comprehensive insights it offers, capsule endoscopy holds promise as a diagnostic tool, especially for patients who cannot undergo traditional endoscopy.
This case report details the application of capsule endoscopy in a Shih Tzu patient with acute hemorrhagic vomiting, demonstrating its utility and potential implications in future clinical practice.
CASE REPORT
A 14-year-old castrated male Shih Tzu presented with acute hemorrhagic vomiting (hematemesis; Fig. 1A) at the Gyeongsang National University Animal Medical Center (GAMC). Three days prior to presentation at the GAMC, the patient was admitted to a local animal hospital following an abrupt onset of hematemesis. The client speculated that this sudden hematemesis may have resulted from a recent switch to an affordable diet. Although the dog underwent intensive treatment at a local animal hospital and showed marginal improvement, it was referred to us for precise diagnosis and targeted treatment.

Upon physical examination, the dog had a slightly elevated body temperature within the normal range (38.9°C). The respiratory and heart rates were within normal limits. Notably, auscultation of the heart revealed a grade 4/6 murmur in the left apex.
Blood tests revealed increased levels of symmetric dimethylarginine (21 μg/dL; reference range: 0–14 μg/dL) and creatinine (1.9 mg/dL; reference range: 0.5–1.8 mg/dL). All the other blood parameters were normal.
Radiographic examination of the thorax revealed bulging of the right and left atria, left ventricle enlargement, left main bronchus compression, and dorsal elevation of the thoracic trachea. In contrast, the abdominal radiographs showed no abnormalities. However, abdominal ultrasound revealed mild thickening of the pyloric wall, measuring 7.0 mm, along with the loss of distinct wall layers.
The owner was aware of the patient’s cardiac condition based on a previous evaluation at a local animal hospital (myxomatous mitral valve disease ACVIM stage B2) and did not want the dog to further undergo echocardiography in our hospital.
Based on the clinical signs and data, GI endoscopy is recommended as the most informative approach to pinpoint the cause of acute hemorrhagic vomiting in dogs. However, considering the patient’s unevaluated cardiac status and potential associated risks, the client decided against any procedure requiring anesthesia.
To address these concerns and offer a less-invasive diagnostic modality compared to other feasible options, we proposed capsule endoscopy, which is an anesthesia-free method. After obtaining the owner’s consent, we proceeded with the capsule endoscopy examination (MiroCam®, MC1200-M, IntroMedic, Seoul, Korea; length: 24.5 mm, diameter: 10.8 mm; Fig. 1B). Prior to undergoing capsule endoscopy, the patient was subjected to a 12-hour fasting period, although water was made accessible. Simethicone (20 mg/dog) was administered 20 minutes prior to the procedure to minimize gastric gas, thereby facilitating improved capsule endoscopy imaging. Electrodes for capsule endoscopy were then affixed, followed by oral administration of the capsule endoscope.
The capsule endoscopy procedure, encompassing the esophagus, stomach, small intestine, and large intestine, took approximately six hours (Fig. 1C). The examination results highlighted pronounced redness and thickening of the gastric mucosa, along with some bleeding (Fig. 2). In contrast, all other parts of the GI tract (esophagus, small intestine, and large intestine) appeared normal based on the capsule endoscopy findings.
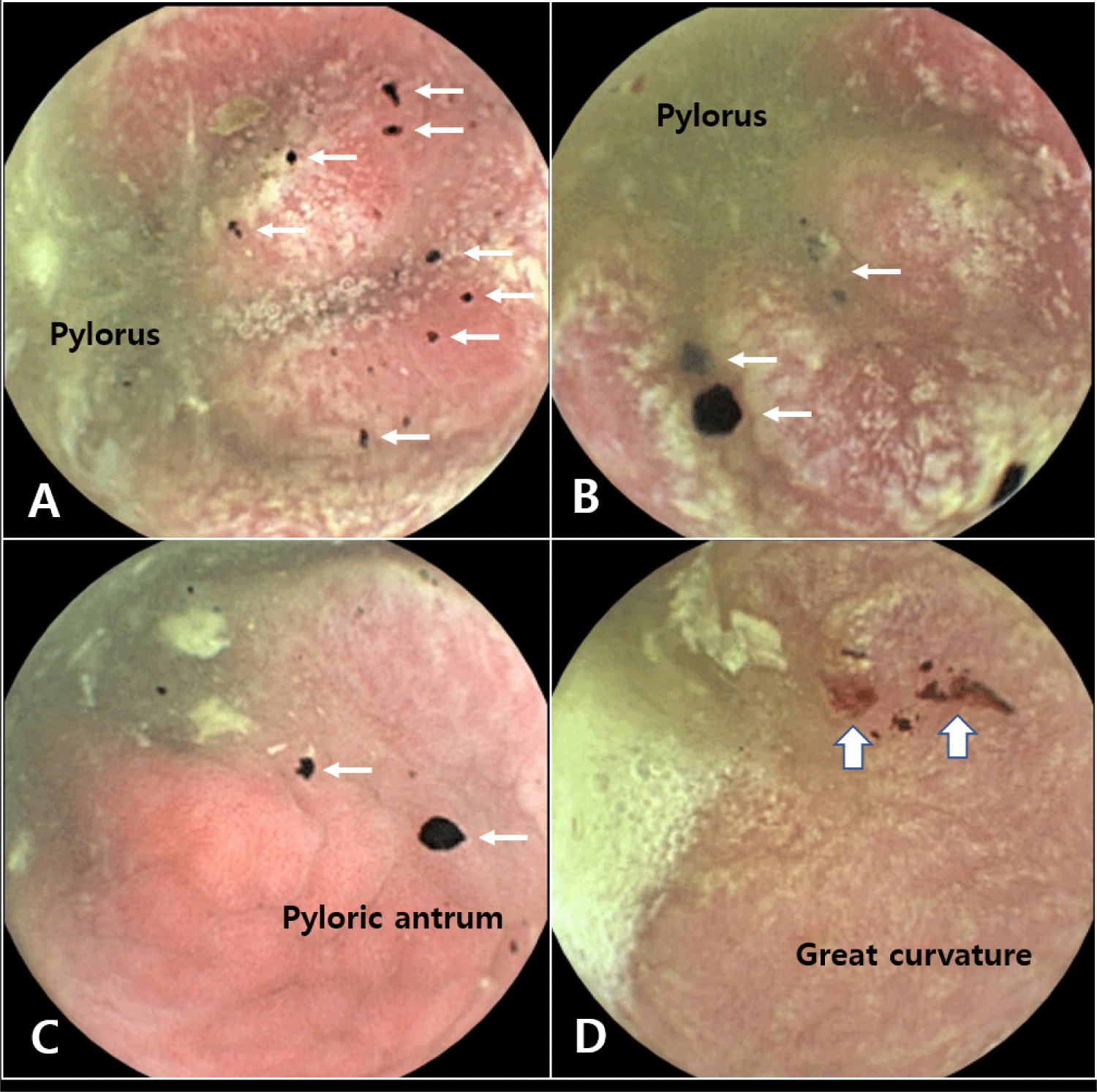
Based on these capsule endoscopy observations, the patient was tentatively diagnosed with severe acute gastritis. As a result, we prescribed a hypoallergenic diet (Anallergenic®, Royal Canin, Aimargues, France) and omeprazole therapy (Omed®, SK Chemical, Seongnam, Korea; 1 mg/kg PO q12h). Following this targeted treatment, the patient demonstrated gradual alleviation of clinical symptoms.
Follow-up capsule endoscopy was scheduled and conducted three weeks after treatment. The findings, when compared to the initial results, showed a notable decrease in gastric mucosal redness and thickening with no bleeding (Fig. 3). Based on the encouraging capsule endoscopy results and marked improvement in clinical symptoms, omeprazole administration was continued for an additional three weeks before discontinuation. However, the transition to a hypoallergenic diet has been maintained as a long-term dietary management strategy.
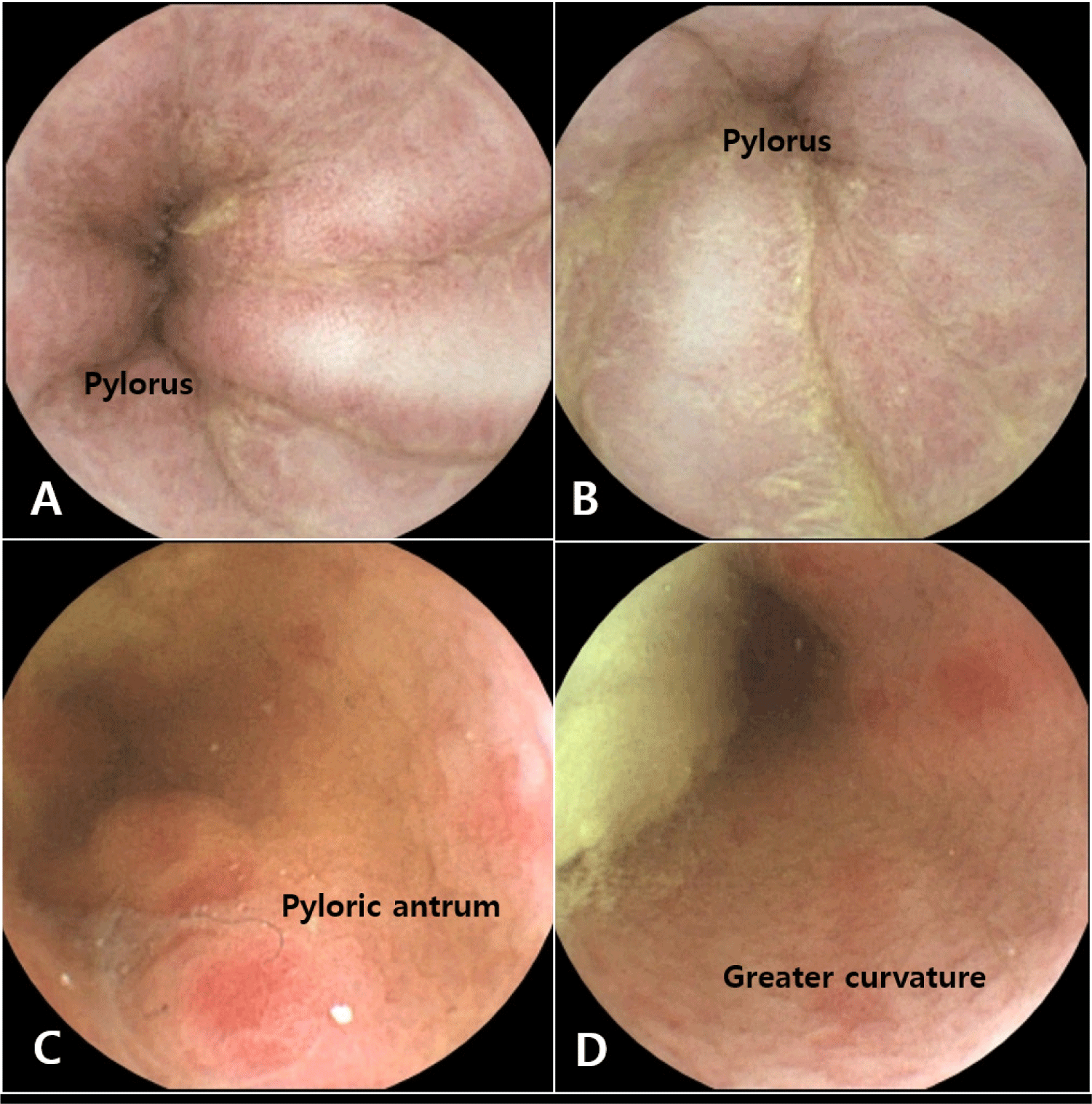
DISCUSSION
Gastritis, defined as the inflammation of the gastric mucosa, presents with a spectrum of clinical signs, with hematemesis being among the most clinically concerning [1, 2]. Etiology of gastritis in dogs is complex and encompasses factors ranging from dietary indiscretion to systemic illness [1, 2]. In this case, the temporal relationship between the onset of symptoms and the switch to a more economical diet suggests that potential dietary irritants or even contaminants are causal factors.
Diagnostic modalities, such as abdominal ultrasonography offer valuable preliminary insights, as evidenced by the identification of gastric wall thickening in this patient. However, the definitive characterization of mucosal inflammation and bleeding often necessitates direct visualization.
Traditionally, GI endoscopy is the modality of choice for such visualization [3, 4]. Its limitations become apparent when anesthesia poses a significant risk, especially in patients with concomitant health concerns. In our patient, the Shih Tzu with a known heart murmur, the risks associated with anesthesia were considered contraindications to traditional endoscopy.
Capsule endoscopy, a newer veterinary diagnostic tool, offers a noninvasive alternative [5–9]. Its utility, as demonstrated in this case, lies in its ability to provide a detailed assessment of the GI tract without the need for anesthesia, particularly in high-risk patients.
The initial findings of capsule endoscopy, characterized by marked mucosal erythema, mucosal thickening, and hemorrhage allowed for a presumptive diagnosis. A follow-up study validated the therapeutic interventions and demonstrated a notable reduction in the inflammatory status. Relative to the initial capsule endoscopy evaluation, there was a marked reduction in the erythema of the gastric mucosa, and neither active bleeding nor blood clots were detected. These findings align with the current literature emphasizing the value of capsule endoscopy for both diagnostic accuracy and therapeutic monitoring [5–9].
The management of this patient, encompassing dietary modifications and omeprazole administration, highlights a holistic approach to diet-induced gastritis [1, 2]. While treating evident inflammation is paramount, addressing potential triggers, such as dietary factors, is equally critical. The positive clinical trajectory observed postintervention supports this multifaceted therapeutic strategy.
One limitation of the present case is that the diagnosis was not substantiated through biopsy and histopathological examination. While capsule endoscopy has the limitation of not permitting biopsy, it offers the distinct advantage of enabling provisional diagnosis of GI tract diseases without the need for anesthesia.
In summary, this case highlights the necessity for adapting diagnostic strategies in veterinary medicine. With the evolving landscape of available tools, modalities, such as capsule endoscopy, can bridge the gap between diagnostic necessity and patient safety. As the field progresses, such innovations underscore the trajectory toward more tailored and patient-centric care paradigms.







