Introduction
Canine pyometra, also known as cystic endometrial hyperplasia complex, is a disease of the uterus in intact female. Sexually mature bitches usually diagnosed from 4 weeks to 4 months after estrus [1-3]. It affects nearly one fourth of all female dogs before they reach ten years of age [4,5]. Many studies indicate an increased incidence of pyometra in nulliparous bitches and in bitches over 4 years of age [3,6].
The endometrial hyperplasia is induced by progesterone and is normally observed before the occurrence of pyometra [6,7]. The bacterial infection is a secondary condition [6,8]. Bacteria ascend through the cervix and into the uterus during estrus [7]. One microorganism normally associated to this disease is E. coli [8,9].
Bitches with pyometra may present either with a vaginal discharge present [open-cervix pyometra] or without a vaginal discharge [closed-cervix pyometra]. Common clinical signs include vulvar discharge, lethargy, depression, inappetence, polyurea, polydypsia, vomiting, diarrhea and abdominal distention. Bitches with closed cervix pyometra generally are very ill at present, death may occur due to toxemia alone or may be associated with peritonitis due to rupture of uterus [1, 4, 10, 11].
The opening in Fallopian tube into the uterus is called the uterine ostium. Uterotubal junction controls the passage of the sperm into oviduct and embryos into the uterus. Also, this junction prevents backflow of debris during parturition or menstruation [12]. In normal cases, uterotubal junction prevent pus leaking into the abdomen during pyometra. The present case report is to describe that uterine pus was leaked into abdominal cavity through oviduct in a Siberian husky with pyometra.
Case report
A 7-year-old, Siberian husky was presented to the Veterinary Medical Center of Chungbuk National University with vomiting and diarrhea after a fight with cohabiting dog. Initial diagnostic evaluation included physical examination, radiography, abdominal ultrasonography and laboratory examination. 10% dehydration was observed.
On electrolyte examination, Na and Cl ions were lower than normal values, and Ca ion was slightly lower than normal values (Table 1). On blood chemistry examination, blood urea nitrogen (BUN) and alkaline phosphatase (ALP) value were extremely higher than normal values (Table 1). Increasement of segmented neutrophils was revealed on complete blood count (Table 2).
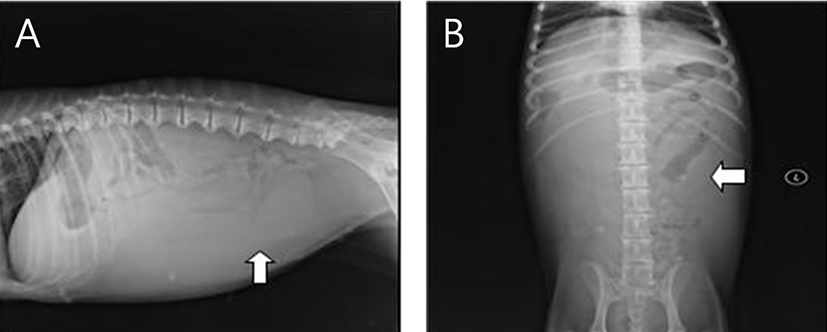
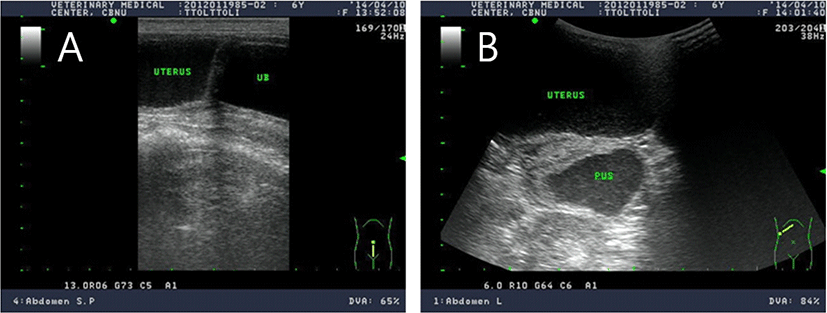
A radiographic examination, from urinary bladder to liver, revealed a pipe shape structure with a radius up to 4 cm (Fig. 1). On ultrasonography, enlarged uterine body was observed. Uterus was enlarged and filed with echogenic fluid that is seemed to be pus. Uterine body was rubbing against the bladder (Fig. 2).
Based on the laboratory examination, radiography and ultrasonography, we finally diagnosed closed-cervix pyometra. The patient was anesthetized by inhalation method for surgical treatment. For induction of anesthesia, propofol (Provive Inj®; 10 mg/mL, Myungmoon Pharm, Korea) was administered intravenously until lack of jaw tone, lack of gagging reflex and coughing reflex. After induction, anesthesia was maintained with isoflurane (Terrell™, Piramal Critical Care, Bethlehem).
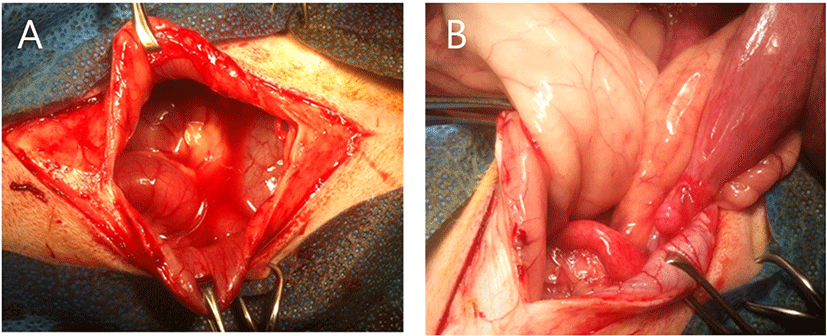
At laparotomy, uterine body and horn were enlarged. Abdominal cavity was filled with mixture of pus and ascite. On area of the left uterine horn, pus leakage was observed (Fig. 3). First, ovariohysterectomy was performed with routine method. And then, abdominal flushing was performed 5 times and suction it. The mixture of pus and ascites was collected for susceptibility test of antibiotics and bacterial identification as soon as abdominal incision.
As postoperative treatment, we prescribed tramadol (3 mg/kg, IV, TID), cefazolin (30 mg/kg, IV, QID), ampibactam (22 mg/kg, IV, QID), famotidine(0.5 mg/kg, IV, BID), metronidazol (10 mg/kg, IV, BID), Vit B (0.5 mL/body, IV, BID), taurine (5 mL/body, IV, BID) and heparin (100 IU/kg, SC, TID).
From antibiotics susceptibility test, cefazolin, cefotaxime, gentamycin and ciprofloxacin showed susceptibility. Doxycycline, amikacin and piperacillin-tazobactam showed intermediate susceptibility and trimethoprim-sulfazine, clarithromycine and tetracycline showed resistance(Table 3).
For bacterial identification, the uterine and abdominal fluid were spread in 5% sheep blood agar, then incubated during 24 h at 37°C. After 24 h, the colony morphology was smooth, mucoid, non-hemolytic and hemolytic. Also, on molecular diagnosis test, both samples from uterine and ovary was confirmed to be E. coli.
Discussion
Pyometra is characterized by bacterial infection and inflammation with pus accumulating in the uterus in combination with cystic illness [1, 4, 13]. The disease is regarded as an emergency because early diagnosis and rapid therapeutic intervention are necessary to prevent a fatal outcome [7, 13, 14]. The safest and most effective treatment is ovariohysterectomy which is performed as soon as the general condition is stabilized [10,13]. Pure medical treatment is sometimes an option to preserve fertility, but with the risk of progressing illness as long as the infection remains in the body. Recurrence of the condition after treatment is also possible because the uterus might be predisposed for infection [14-17].
In this case, dog had been diagnosed as a closed-cervix pyometra. After surgery, we prescribed cefazolin for antibiotics. From molecular diagnosis test, E. coli was confirmed. Fransson et al [18] isolated a 90% rate of E. coli in bitches with pyometra. Coggan et al [6] isolated a 76.6% of E. coli in bitches with pyometra. Oluoch et al [9] studied 674 strains of E. coli and observed 90% sensitivity in norfloxacin, 87.5% to enrofloxacin, 90.7% to gentamicin and 85.9% to amicacin. Coggan et al [6] studied 151 strains of E. coli and observed 86.1% resistance to cephalothin and 68.9% to ampicillin. Also observed 94% sensitivity to norfloxacin, compare to 75.5% in enrofloxacin, 70.2% in gentamicin, 55.6% in amicacin. In our case, pathogen was susceptible to cefazolin, cefotaxim, gentamycin, ciprofloxacin and resistance to clarithromycin, trimethoprim_sulfazine and tetracyclin. That means that various strains of E. coli can induce pyometra.
Dogs with pyometra was closed by the uterine cervix and ovarian tubal junction because they are in diestrus restrained by progesterone. Therefore, in a general condition, it is very rare that an abscess in the uterus enters the abdominal cavity through the oviduct [2,19]. However, there is a report that the uterine rupture or pus leakage into abdominal cavity through oviducts with a large amount of pus accumulated in the uterus [12,19]). The present case also showed vomiting and diarrhea after fighting with cohabiting dog. Ultrasonography confirmed the presence of pus in the abdominal cavity. It was also confirmed that E. coli was the same bacterium that caused pyometra and bacteria isolated from the abdominal cavity.
E. coli was a vast majority of the bitches with a diagnosis of pyometra [18]. An increase in white blood cell and ALP, and toxin degeneration of neutrophil granulocytes can cause gram-negative uterine condition [18,20]. In this case, an incre ase in neutrophil and ALP was confirmed, and E. coli was identified as a causative agent of pyometra. The increase in BUN was also due to the effect of E. coli-derived endotoxin on the kidney.
In conclusion, this case is to describe that uterine pus was leakage into abdominal cavity through oviduct in a Siberian husky with pyometra, and pus leakage from uterus may be cause septic peritonitis and death. Also, this case must be considered that physical event such as fight against cohabiting dog, strenuous exercise and kiss-off can cause uterine rupture or pus leakage through oviduct from uterus in dog with pyometra.







