Introduction
Lymphoma is among the most frequently diagnosed malignancies, and represents the most commonly managed neoplasia in dogs [1, 2]. Canine lymphoma is classified as either multicentric, gastrointestinal, mediastinal, or cutaneous based on the anatomical location [3]. Among them, mediastinal lymphoma accounts for approximately 5% of cases, although this patient population has not been well described due to its rare incidence in veterinary medicine [3].
Mediastinal lymphoma can either be of the T-cell or B-cell phenotype [4, 5], but the most commonly encountered form of primary mediastinal lymphoma is of the T-cell phenotype, based on the limited information in dogs [6]. T-cell lymphoma shows a generally poorer outcome compared to B-cell lymphoma, despite the fact that multidrug chemotherapy [6, 7] with progression-free survival (PFS) and overall survival (OS) is reported to range from 96 – 200 days to 120 – 270 days, respectively [8, 9], thus primary mediastinal lymphoma might have a poor outcome. R-CHOP (cyclophosphamide, doxorubicin, vincristine, and prednisone, plus rituximab) is the most commonly used chemotherapy, but dose-adjusted EPOCH-R (etoposide, prednisone, vincristine, cyclophosphamide, and doxorubicin, plus rituximab) is also considered in humans with PMBL, and both have good therapeutic responses [10, 11].
Canine primary mediastinal lymphoma has not yet been well described [6]. It is characterized by nonspecific clinical signs, including respiratory disorder, polydipsia/ polyuria, vomiting, and T-cell phenotype, which is a factor that causes a worse outcome than B-cell phenotype [12, 13]. In a previous study, treatment with a CHOP (cyclophosphamide, doxorubicin, vincristine, prednisone)- based protocol was associated with an improved PFS (144 days) and OS (194 days) when compared with another protocol [6], but the study had too small a number of dogs receiving each other protocol to accurately compare the efficacy of the CHOP protocol, thus there is still a lack of information on the efficacy of multidrug chemotherapy, including the CHOP protocol, in canine primary mediastinal lymphoma. Subsequently, the purpose of this case report is to describe a case in which PMBL had a favorable response to L-CHOP chemotherapy without any recurrence of tumors.
Case Report
A one-year-old intact female Maltese weighing 2.12 kg was presented with anorexia and regurgitation. The dog was lethargic and tachypneic (respiratory rate of 96 breathes per minute). The pulse rate was increased (212 beats per minute) and femoral pulse quality was normal at palpation. The peripheral lymph nodes were not palpably enlarged. Other findings of the physical examination were unremarkable. Complete blood counts were within normal limits. The serum biochemistry panel findings were unremarkable, except for increased serum alkaline phosphatase activity (198 IU/L; reference interval [RI], 29 − 97 IU/L).
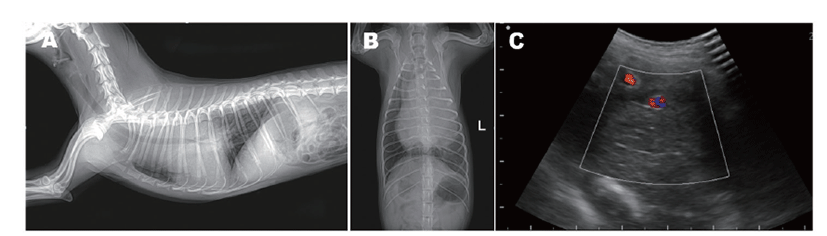
In survey radiographs, there was a soft tissue opacity in the left cranial mediastinum (Fig. 1) as well as a displacement of the trachea to the right on dorsoventral and ventrodorsal radiographs. On right lateral radiographs, there was a well-defined 3.6 × 4.0 (width × height) cm circular soft tissue located between the 3rd and 6th ribs of the ventral margin (Fig. 1A). In the ventrodorsal radiographs, a 1.5 × 2.3 (width × height) cm mass of soft tissue was observed in the region of the caudal dorsal part of the tracheal bifurcation, which was presumed to be a tracheobronchial lymph node (Fig. 1B). In ultrasonographic images of the cranioventral mediastinum, a homogenous mass of moderate echogenicity surrounding mediastinal vessels including aorta was observed (Fig. 1C). The abdominal ultrasonography meant to evaluate metastasis showed no abnormal lesion.
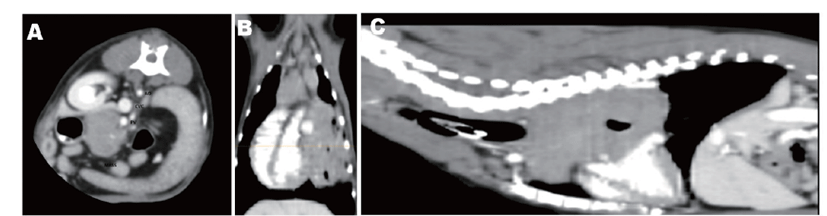
Computed tomography images of the thorax were taken under general anesthesia at second presentation in order to determine the origin of the mass and the decision of surgical resection. The size of the mass was measured at 5.2 cm × 4.7 cm × 7.1 cm (width × height × depth), and it was mostly diffusely expanded in the thoracic inlet to the left hemithorax and caudodorsal mediastinum. The mass was in contact with the left side of the heart, compressing the heart and trachea while shifting mediastinum to the right, and the cranial part and caudal part of the left lobe were collapsed by the mass (Fig. 2A). Significant displacements of the major cranial mediastinal blood vessels, cranial vena cava, and thoracic aorta were also observed, but invasion was not. The caudal vena cava was partially compressed at the level adjacent to the heart base (Fig. 2B). The distinction between mass and cranial mediastinal lymph node was ambiguous. An enlarged bilateral sternal lymph node with an oval to round shape on the back of the first sternum was confirmed which exhibited a well-defined, irregular marginated, and heterogeneously moderate contrast-enhancing pattern (Fig. 2C). The decision on surgical resection could not be made due to the location as well as the ambiguous distinction between mass and cranial mediastinal lymph node.
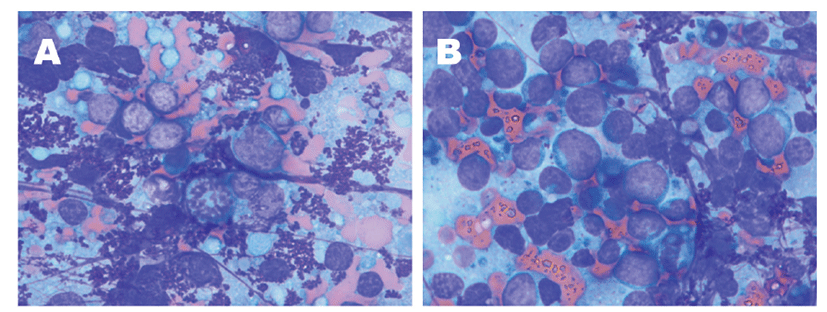
Fine-needle aspiration was performed from the mediastinal mass for cytology immediately following computed tomography scan. On cytology, the majority of the cells were lymphocytes, small 40%−60% and medium to large 40%−60%. The mitotic index was observed at 3/5 hpf (Fig. 3A and B). In addition, a number of cells with refractory granules in the cytoplasm were observed, and these were presumed to be Mott cells or plasmacytoid cells. Based on the increased rate of immature lymphocytes and the high mitotic index, it was likely to be a large-cell lymphoma. However, the rate of lymphocyte was somewhat ambiguous, and the possibility of reactive hyperplasia could not be ruled out in consideration of the observation of the Mott cell. Polymerase chain reaction for Antigen Receptor Rearrangement (PARR) assay was performed for definitive diagnosis, and the result indicated B-cell lymphoma with the clonal peak of the IgH gene. PMBL was subsequently confirmed. Based on the World Health Organization’s clinical staging system for lymphoma in domestic animals, the dog was classified as stage 1b, due to only mediastinal involved with systemic signs such as regurgitation, lethargy, and anorexia.
To date, there has been no standardized chemotherapy for primary mediastinal lymphoma in the veterinary literature. In general, it is recommended that surgery can be considered for those cases where the disease is shown to be localized, but the site as well as the distinction between mass and lymph were ambiguous, so systemic therapy was chosen. The dog showed the World Health Organization’s stage 1 lymphoma, which has a better prognosis than the more advanced stages, and B-cell phenotype, which is associated with significantly longer remission and survival duration compared to T-cell phenotype following CHOP-based protocols in canine multicentric lymphoma [6]. Based on these facts, treatment was initiated using L-CHOP, also known as the modified 25-week University of Wisconsin-Madison (UW-25) chemotherapy protocol [14], which includes L-asparaginase, cyclophosphamide, doxorubicin, vincristine, prednisolone. Follow-up examinations including standard haematological parameters, serum chemistry profile, and radiographic evaluations were performed every week of chemotherapy treatment. Ultrasonographic examination was performed monthly for the detection of metastasis in other organs or for the evaluation of tumor remission. All tumor-associated clinical symptoms subsided after the first chemotherapy treatment. This initial treatment resulted in complete tumoral remission (Fig. 4A and B).
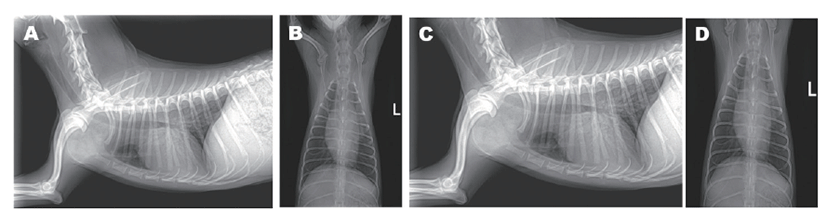
On week 4, the dog showed a high rectal temperature (39.5℃), neutropenia (430 cells/μL, RI, 2,950 – 11,640 cells/μL), and anemia (packed cell volume = 29.2%, RI, 37.3 – 61.7%), therefore the fourth chemotherapy treatment was postponed. There was no evidence of infection based on the other physical examination and blood analyses results, but cefotaxime sodium (30 mg/kg IV q 12 h), a prophylactic antibiotic, was administered with fluid therapy. The following morning, rectal temperature was normalized and there were no other abnormal signs. The dog was discharged with medications including cephalexin (30 mg/kg PO q 12 h). Chemotherapy resumed the following week, it continued without any delay, and the dog remained in complete remission from the termination of chemotherapy treatment (Fig. 4C and D) through to week 72, the last on-call confirmation.
Discussion
In dogs, the outcome of primary mediastinal lymphoma may be consistent with multicentric high-grade T-cell lymphoma, because the T-cell phenotype is most often associated with primary mediastinal lymphoma in dogs [12]. There has only been one cohort study for canine primary mediastinal lymphoma, and that study only included one case of B-cell phenotype, implying there has been little information on the B-cell phenotype in canine primary mediastinal lymphoma. The previous study also showed that the median PFS and OS for dogs treated with CHOP-based multi-agent chemotherapy were 144 and 194 days [12], respectively, but this may also represent cases of the T-cell phenotype. Therefore, there has been no available data about PMBL in dogs treated with CHOP-based chemotherapy. Above all else, standardized chemotherapy protocols have not been established for PMBL in humans and dogs [12], but CHOP-based chemotherapy protocols with or without radiation therapy are generally recommended in humans with PMBL [10]. In the present report, a dog with PMBL was treated with the L-CHOP protocol based on the phenotype and the efficacy in canine multicentric lymphoma [14, 15], and the dog has since been alive for more than 540 days after the completion of chemotherapy without relapse. To the best of our knowledge, this is the first case report of canine PMBL treated by CHOP-based chemotherapy. Therefore, this report presents an available treatment option for primary mediastinal lymphoma in dogs.
In the present report, the age of the case was somewhat young compared to the previous study examining dogs with primary mediastinal lymphoma (mean age, 7.8 years; range 2.5 – 12.1 years). According to reports in humans, patients with PMBL are typically young, with a slight to moderate female patient prevalence, compared to patients with other subtypes of DLBCL [16, 17]. Unlike the case of multicentric lymphoma, which is well known to occur in middle-to-old age, the case in the present report was of an intact female at an early age, suggesting that the clinical features of this disease in humans might be similar in dogs.
Previous publications have reported that dogs with mediastinal masses in the multicentric lymphoma disease setting have a worse prognosis than dogs without mediastinal involvement; however, these studies did not evaluate the phenotype [6]. When subsets of patients with a T-cell phenotype have been evaluated, mediastinal involvement has not been reported to be a negative prognostic factor [6]. Therefore, there seems to be a limit to evaluating the prognosis or therapeutic response based only on the anatomical location of the lymphoma in the dog, and thus a comprehensive evaluation of histologic classification including morphologic and immunophenotypic features of the corresponding lymphocyte should be performed. In addition, considering the case described herein, the factor that had the greatest impact on the patient’s prognosis was the histologic, immunophenotypic features of the lymphocytes (B-cell phenotype) that constituted it, rather than the anatomical location of the mass.
The B-cell immunotype is a positive prognostic factor in lymphoma, and high-grade lymphoma is known to be a negative prognostic factor, but one that responds well to chemotherapy [18, 19]. Therefore, since the dog described herein was B-cell immunotype, it was able to survive beyond the reported survival period without symptoms of recurrence. In addition, because the dog was classified as having high-grade lymphoma representing the ratio of medium to large cells as 40%−60%, it seemed to achieve a good therapeutic response close to complete remission immediately following the initial treatment.
The chemotherapy drugs included in this protocol were chosen based on their proven efficacy, as known by its use in multicentric lymphoma. In human medicine, however, patients with PMBL are treated by a CHOPbased chemotherapy regimen using rituximab [4, 20]. In the present report, the L-CHOP protocol was safely applied in a dog with PBML, but it is unclear if a different multidrug protocol (e.g. L-MOPP, where L stands for L-asparaginase, M for mechlorethamine, O for vincristine, P for procarbazine, and P for prednisone) would have resulted in a better or similar outcome, and larger studies are needed to assess the efficacy of various other chemotherapy protocols in treating canine primary mediastinal lymphomas. However, the rapid improvement in clinical signs and result of treatment was sufficiently encouraging to consider it to be a first-choice option for the treatment of canine primary mediastinal lymphoma.
The L-CHOP protocol has been shown to be well tolerated in dogs, where 41.5% of dogs required at least one dose reduction or delay at some point in the chemotherapy [14]. In particular, the toxicity of L-CHOP mostly occurred following vincristine administration [14]. The chemotherapy in this case was also delayed once on week 4, which was one week following vincristine treatment, due to high rectal temperature, neutropenia, and anemia. Fortunately, there was no evidence of infection, and the rectal temperature was stabilized after the administration of prophylactic antibiotics with fluid therapy, and chemotherapy resumed one week later without any delays.
In conclusion, the case described herein showed complete tumoral remission with L-CHOP chemotherapy, and the chemotherapy was safely applied. Clinicians should be aware that the clinical response and prognosis can be good in canine PMBL treated with the L-CHOP protocol, as is already known in human patients.







