Introduction
Feline eosinophilic granuloma complex, which is characterized by a group of lesions affecting the skin, mucocutaneous junctions, and oral cavity, is a common in- flammatory skin disease in cats. Although the etiology of this condition is unknown, the histological appearance of lesions suggests an immune-mediated mechanism, possibly a hypersensitivity reaction to an unknown antigen [1,2,3,12,15,16,17,18,19]. Classically, three types of lesion have been characterized in feline eosinophilic granuloma complex: (1) the indolent ulcer, (2) the eosinophilic plaque, and (3) the eosinophilic granuloma [3,4,5]. In particular, eosinophilic granulomas occur on the caudal thighs, cheek, and oral cavity. The oral lesions can occur anywhere in the mouth, including the gingiva, hard and soft palates, oral and nasal pharynx, and tongue; occasionally, lesions even manifest in the draining lymphoid tissues [2,3,6]. Lesions in the oral cavity and on the face have a papular to nodular configuration [3], and cats with oral lesions may be dysphagic [1,2,6]. In addition, eosinophilia may occur in the blood, especially when oral lesions are present [2,3].
Tacrolimus is an immunosuppressive antibiotic of the macrolide family; it is 10- to 100-fold more potent than cyclosporine in the inhibition of T-cell activation [7,8,20]. The agent works by inhibiting calcineurin, a calcium-activated protein phosphatase, that is necessary for appropriate immune modulation [9]. A topical formulation of tacrolimus has been reported to be efficacious in the treatment of canine atopic dermatitis [10], but few efficacy and safety reports exist in the veterinary literature.
Case report
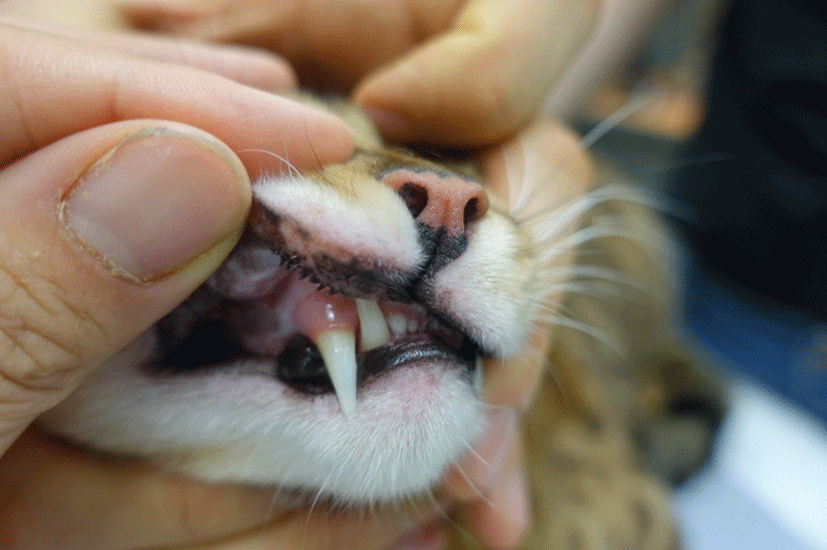
A spayed male Bengal cat showing swelling and redness in the lips and gingiva was referred to the department of veterinary internal medicine, Chonnam National University. Upon physical examination, swelling and redness on the upper and lower lips were found (Fig. 1). Futhermore, well-circumscribed, raised, and pink lesions were found in the oral cavity. In general, the lesions on the lips and gingiva were well-circumscribed and not ulcerative.
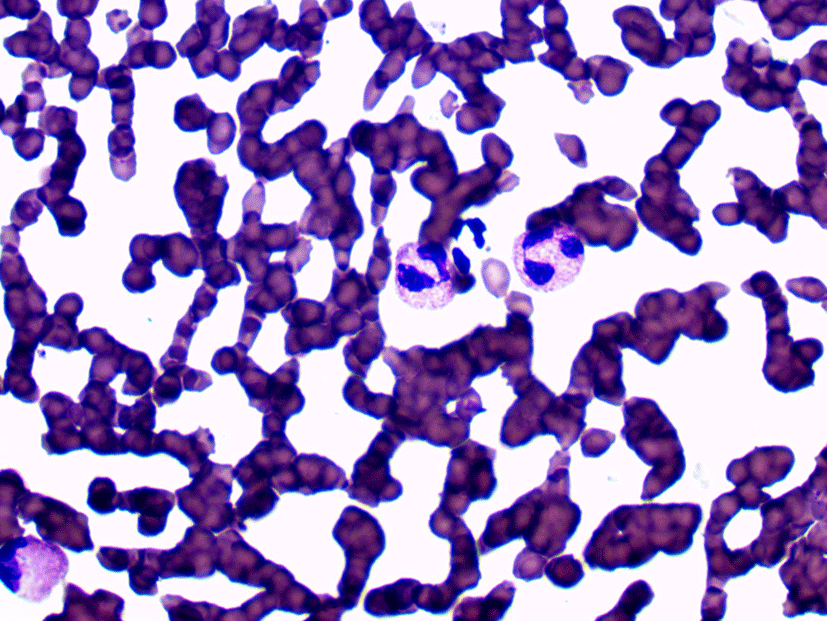
There is no remarkable findings on Complete blood counts (CBC) and serum biochemistry profiles. Direct microscopy of cutaneous lesions was performed, using impression smear technique. Cytological examination of the lesions showed numerous eosinophils (Fig. 2). Bacterial and fungal cultures of the lesion in the oral cavity were negative.
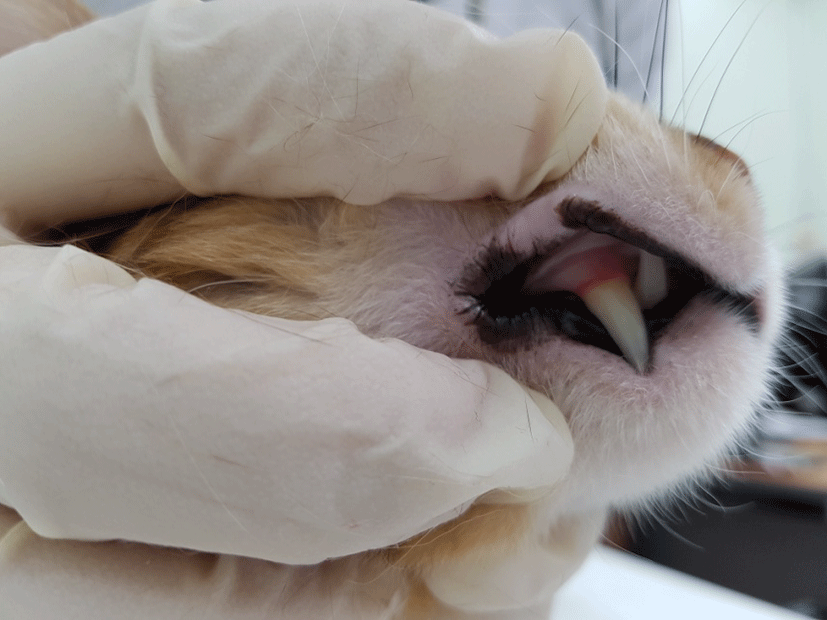
Based on the clinical appearance and cytology, eosinophilic granuloma was diagnosed, and the lesions were initially treated using prednisolone (PDS; Solondo®; 1 mg/kg, p.o, bid; Yuhanyanghaeng, Seoul, South Korea) with cyclosporine (Cipol-N®; 5 mg/kg, p.o, sid; Jonggeundang, Seoul, South Korea) because the patient’s history showed that a similar lesion had relapsed when treated using PDS-only therapy. At the next visit, the cyclosporine was withdrawn due to severe vomiting. PDS-only sole therapy was maintained for 2 month, with gradual tapering, before being discontinued. One month later, however, the lesion had relapsed. Because of the recurrent relapse of the lesion, a new combination therapy was initiated; oral tacrolimus (Advagraf®; 0.3 mg/kg, p.o, bid; Astellas Pharm. Co., Netherlands) with PDS (Solondo®) was administered. The clinical signs improved gradually over the course of 1 week (Fig. 3). The tacrolimus was gradually tapered for 1 month, and the PDS was gradually tapered for 4 months. The oral lesion had not relapsed after 3 months of follow-up.
Discussion
The cat in this report was administered immunosuppressive therapies to treat eosinophilic granuloma. As an initial treatment, oral PDS with cyclosporine was administered. Several mild adverse events have been related to cyclosporine use in cats (salivation, vomiting, headshaking, intermittent soft feces, and gingival hyperplasia) [11]. In the present case, the cyclosporine was stopped due to vomiting.
Subsequently, PDS was combined with a new, trial formula of tacrolimus for 1 month, and the treatment showed efficacy in this case. The erythema and swelling of the lips and gingiva improved rapidly. Tacrolimus belongs to an important class of immunomodulators known as calcineurin inbibitors, which also include cyclosporine [13]. Calcineurin inhibitors also inhibit the activation of mast cells, basophils, eosinophils, keratinocytes, and Langerhans cells [13]. Both cyclosporine and tacrolimus decrease the number and activity of epidermal dendritic cells and down-regulate the expression of the high-affinity immunoglobulin E receptor on Langerhans cells [13]. Although similar to cyclosporine in its mechanism of activity, tacrolimus is structurally different [13]. Moreover, the potency of tacrolimus has been estimated at 10 to 100 times greater than that of cyclosporine [13]. More recently, additional applications have been reported, including treatment of actinic dermatosis, psoriasis, and the early stages of cutaneous T cell lymphoma [13].
There is no standard protocol for the investigation and treatment of feline eosinophilic granuloma. Systemic treatment using other immunosuppressants that act on T cells (e.g. cyclosporine or glucocorticoids) is the only reported recommendation. Although PDS is fast and effective in the treatment of eosinphilic granuloma in cats, long-term systemic glucocorticoid treatment can lead to adverse glucocorticoid-induced effects. Furthermore, in the present case, severe eosinophilic granuloma relapsed after PDS tapering. Therefore, the combination of PDS and tacrolimus was a good choice in the present case, because the recurrent relapses stopped.
In contrast, in human patients undergoing solid organ transplant, tacrolimus induces thrombocytopenia [14]. Therefore, the use of tacrolimus in feline eosinophilic granuloma should be investigated in more cases.
In conclusion, the present case indicated that the combination of PDS and tacrolimus is effective for reducing relapse in feline eosinophilic granuloma. To our knowledge, this is the first report to successfully combine tacrolimus with PDS in the long-term treatment of feline eosinophilic granuloma.







