ARTICLE
Usefulness of COPD Assessment Test as valuable predictor of depression in chronic obstructive pulmonary disease
Sei Jin Youn, Mi Kyeong Kim, Jin Young An*
Author Information & Copyright ▼
Department of Internal medicine, College of Medicine, Chungbuk National University, Cheongju 28644, Korea
*Corresponding Author : Jin Young An Department of Internal medicine, College of Medicine, Chungbuk National University, Cheongju 28644, Korea Tel: +82-43-269-6308, Fax: +82-43-269-6069,
drahnjy@chungbuk.ac.kr
© Research Institute of Veterinary Medicine, Chungbuk National University All rights reserved. This is an Open-Access article distributed under the terms of the Creative Commons Attribution Non-Commercial License (http://creativecommons.org/licenses/by-nc/3.0/) which permits unrestricted non-commercial use, distribution, and reproduction in any medium, provided the original work is properly cited.
Received: Sep 15, 2015; Revised: Nov 11, 2015; Accepted: Nov 16, 2015
Abstract
Chronic obstructive pulmonary disease (COPD) is associated with multiple comorbidities, including depression, which carries a higher risk of exacerbation and hospitalization in patients with stable COPD. A newly developed questionnaire, the COPD Assessment Test (CAT), was developed as an alternative to other complex, time-consuming tools for quantifying the symptom burden of COPD in routine practice. It is possible that the correlation between the CAT and depression scales could be useful for early evaluation and management of depression in COPD patients. Thus, we investigated the relationship between the CAT and depression as measured by the Patient Health Questionnaires-9 (PHQ-9). We performed a retrospective observational COPD cohort study. A total of 97 patients were enrolled. The Korean versions of the CAT and PHQ-9 were completed for stable patients. A correlation analysis was performed between the PHQ-9 and CAT scores. Significant depression among the groups based on the 2011 GOLD guidelines occurred only in class Gold B and D patients (40% and 60%, respectively). The frequency of depression was significantly higher in the group with higher CAT scores (20~29 versus ≥30; odds ratio: 5.67 versus 22.66). Significant association was observed between the PHQ-9 and CAT scores (r=0.545 and P<0.001). As a result, the PHQ-9 score was significantly higher in COPD patients with a higher CAT score. The CAT is a simple and valuable predictor of depression in COPD patients, and it should be frequently used to detect COPD patients with depression in clinical practice.
Keywords: chronic obstructive pulmonary disease; chronic obstructive pulmonary disease Assessment Test; depression; patient health questionnaires-9; global Initiative for chronic obstructive lung disease
Introduction
Chronic obstructive pulmonary disease (COPD) is characterized by progressive and partially reversible airflow limitation. The prevalence of COPD and associated mortality are increasing worldwide [1, 2]. COPD patients experience a variety of comorbidities, including lung cancer, diabetes, coronary artery disease, osteoporosis, and depression [3, 4]. In stable COPD, the prevalence of clinical depression ranges between 10% and 42% [5, 6]. Depression is associated with higher rates of acute exacerbation, hospital re-admission, and 30-day mortality, in addition to a high economic burden and social problems such as suicide [7, 8]. Although diagnosis of depression in COPD patients can be difficult due to overlapping symptoms between COPD and depression, early detection and appropriate intervention are important [9-11].
The COPD Assessment Test (CAT) is a fairly simple and quick questionnaire. It has good measurement properties and has been shown to be useful for assessing the impact of COPD on quality of life [12, 13]. The aim of the present study was to determine the association between the CAT and depression as measured using the Patient Health Questionnaires-9 (PHQ-9). Therefore, we investigated the CAT score as a predictor of the presence and severity of depression in COPD.
Materials and Methods
Study design
We performed a retrospective observational COPD cohort study at Chungbuk National University Hospital’s outpatient clinics between March and July in 2015. The protocol was approved by the ethics committees of Chungbuk National University Hospital, and a written informed consent was obtained from each patient (2015-02-002).
The main inclusion criteria for the study were as follows: (1) age≥40 years old, (2) forced expiratory volume of 1 sec (FEV1)/forced vital capacity (FVC)<0.7 on the pulmonary function test (PFT), (3) emphysematous changes in the chest X-ray or computed tomography (CT) scans, and (4) chronic respiratory symptoms with a significant history of smoking (≥20 pack-years). The exclusion criteria were as follows: (1) acute exacerbation within the previous 1 month, (2) bronchial asthma or an increase in FEV1 of more than 12% of the predicted value upon use of 400 μg of albuterol, (3) other lung diseases such as bronchiectasis and interstitial lung disease, (4) a history of lung resection surgery, and (5) refusal of consent.
The CAT and PHQ-9 were completed for stable patients by two trained nurses. Upon enrollment, complete medical histories were obtained, and clinical examinations were performed by pulmonary physicians.
Evaluation of COPD
The Korean version of the CAT was validated and used in this study. The CAT is simple to use and indicates a patient’s quality of life. This instrument consists of eight questions, each presented as a semantic 6-point differential scale (0 to 5). Scores of 0~10, 11~20, 21~30, and 31~40 represent a mild, moderate, severe, or very severe clinical impact, respectively [14]. The 2011 Global Initiative for Chronic Obstructive Lung Disease (GOLD) recommends that clinicians use the CAT to assess current symptoms and assign patients to treatment groups based on a CAT scores<10 versus≥10 [15].
Evaluation of depression
The Korean version of the PHQ-9 was used to evaluate depression in COPD patients. The PHQ-9 is widely used in clinical practice to measure severity of depressive symptoms [16, 17]. The PHQ-9 consists of nine questions, and the scores for each item range from 0 (not at all) to 3 (nearly every day) with regard to occurrence of symptoms over the previous 2 weeks. The sensitivity and specificity vary according to the cut-off scores. A score≥10 suggests a high likelihood of major depression. Our study’s cut-off score was 10, as in a previous study by Kroenke et al [18]. The total scores were classified as minimal (0~4), mild (5~9), moderate (10~14), moderate-to-severe (15~19), and severe depression (≥20) [18].
Data analysis
The data are presented as the means ± standard deviation (S.D.). Univariate associations between the PHQ-9 and other variables were analyzed using Pearson’s correlation coefficient. The sensitivity, specificity, positive predictive value (PV), and negative PV of the CAT were calculated. P values less than 0.05 were considered significant. All data were analyzed using the SPSS version 18.
Results
Patient demographics and clinical characteristics
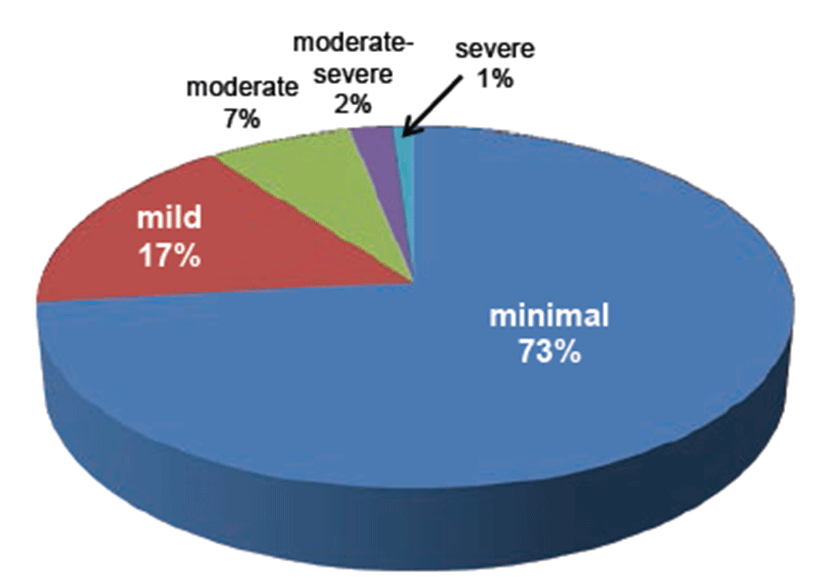
Over a 5-month period, 124 patients with COPD were assessed for their eligibility at an outpatient pulmonary clinic. Of these patients, 97 were enrolled in the study. Basic characteristics of the patients are shown in Table 1. Among the 97 patients, 92% were men. The median age was 67.6 ± 9.3 yr, and the median duration of COPD was 48 months. According to 2011 GOLD recommendations, patients were divided into four groups (A: 10.3%, B: 44.3%, C: 5.1%, and D: 40.3%). The median FEV1 was 59%, and 73.2% were current smokers. The proportion of patients with comorbidities was 22%. Cardiovascular events such as coronary artery disease and cerebral infarct were the most frequent. The mean competence level of inhaler use was 8.42 of 10 points. The median CAT score was 15.2 ± 7.9. Severity of depression was classified as minimal, mild, moderate, moderate-severe, or severe, corresponding to 73%, 17%, 7.0%, 2.0%, or 1.0% of patients, respectively (Fig. 1). The prevalence of significant depression, defined as a PHQ-9 score≥10, was 10.3% (Table 1).
Fig. 1.
Distribution of depression severity by PHQ-9 scores.PHQ-9, Patient Health Questionnarie-9.
Download Original Figure
Table 1.
Clinical characteristics of the study group
| Variables |
Subjects (n=97) |
| Men, n (%) |
89 (92%) |
| Median age, years |
67.6 ± 9.3 (44~85) |
| Median duration of COPD, months |
48 (2~300) |
| Gold stage, n (%) |
|
| A |
10 (10.3%) |
| B |
43 (44.3%) |
| C |
5 (5.1)% |
| D |
39 (40.3%) |
| Median FEV1 (% of predicted value) |
59% |
| Smoking state (n) |
|
| Current smoker |
71 (73.2%) |
| Ex-smoker |
21 (21.6%) |
| Never-smoker |
5 (5.2%) |
| Comorbidities |
|
| Yes (%) |
21 (22%) |
| Cardiovascular event |
10 |
| Arrhythmia |
4 |
| Diabetic mellitus |
3 |
| Hypertension |
4 |
| Cancer |
4 |
| Liver disease |
2 |
| Competence level of inhaler use (0~10) |
|
| Indacaterol |
9 |
| Salmeterol + fluticasone |
8.7 |
| Tiotrotium |
8.5 |
| Formoterol + budesonide |
8.4 |
| Salbutamol |
7.5 |
| Median CAT Score |
15.2 ± 7.9 (1~34) |
| Depression (PHQ-9 score≥10) |
10 (10.3%) |
Download Excel Table
Prevalence of depression according to GOLD stage, CAT score, and comorbidity
Significant depression among the groups based on the 2011 GOLD guidelines was observed in only class Gold B and D patients (40% and 60%, respectively) (Table 2). The frequency of depression was significantly higher in the group with higher CAT scores (20~29 versus≥30; odds ratio: 5.67 versus 22.66). However, the incidence of comorbidity was not correlated with significant depression (Table 3).
Table 2.
Distribution of depression according to GOLD stage, CAT score, and comorbidity
|
|
|
Depression |
|
| No |
Yes |
| GOLD stage |
Mild |
10 (11.5) |
0 (0.0) |
|
|
Moderate |
39 (44.8) |
4 (40.0) |
|
|
Severe |
5 (5.8) |
0 (0.0) |
|
|
Very severe |
33 (37.9) |
6 (60.0) |
| CAT score |
≤9 |
23 (26.4) |
0 (0.0) |
|
|
10~19 |
45 (51.7) |
3 (30.0) |
|
|
20~29 |
16 (18.4) |
4 (40.0) |
|
|
≥30 |
3 (3.5) |
3 (30.0) |
| Comorbidity |
0 |
69 (79.3) |
7 (70.0) |
|
|
1 |
15 (17.2) |
2 (20.0) |
|
|
2 |
1 (1.2) |
1 (10.0) |
|
|
3 |
2 (2.3) |
0 (0.0) |
Download Excel Table
Table 3.
Odds ratio for depression according to GOLD stage, CAT score, and comorbidity
|
|
Depression (PHQ-9 score≥10) |
OR (95% CI) |
| No |
Yes |
| GOLD stage |
Mild to moderate |
49 (56.3) |
4 (40.0) |
1.00 (Referent) |
|
|
Severe to very severe |
38 (43.7) |
6 (60.0) |
1.93 (0.51, 7.34) |
| CAT score |
≤19 |
68 (78.2) |
3 (30.0) |
1.00 (Referent) |
|
|
20~29 |
16 (18.4) |
4 (40.0) |
5.67 (1.15, 27.87) |
|
|
≥30 |
3 (3.5) |
3 (30.0) |
22.66 (3.15, 63.19) |
| Comorbidity |
0 |
69 (79.3) |
7 (70.0) |
1.00 (Referent) |
|
|
≥1 |
18 (20.7) |
3 (30.0) |
1.64 (0.39, 6.99) |
Download Excel Table
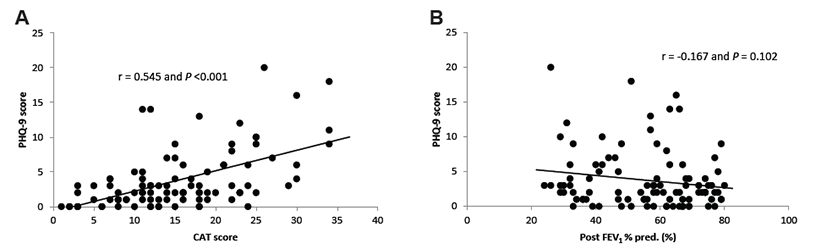
Since patients with significant depression had higher CAT scores, correlation analysis was performed. A significant association was observed between the PHQ-9 and CAT scores (r=0.545 and P<0.001) (Fig. 2), and the PHQ-9 score was significantly higher in COPD patients with a higher CAT score. We also analyzed the relationship between the PHQ-9 score and post-FEV1 and found no significant association (Fig. 2).
Fig. 2.
Scatter diagrams showing correlations between two parameters. (A) Correlation between Patient Health Questionnaire-9 (PHQ-9) and COPD assessment test (CAT). (B) Correlation between PHQ-9 and the Post-forced expiratory volume in 1 second (FEV1).
Download Original Figure
Sensitivity, specificity, and predictive value of CAT score for depression
The capability of the CAT as a predictor of depression was investigated. The sensitivity, specificity, positive predictive value, negative predictive value, and accuracy were calculated according to the CAT score levels. The sensitivity and specificity of a CAT score≥20 were 70 and 78.16, respectively. The accuracy was highest for a CAT score≥30 (Table 4).
Table 4.
Sensitivity, specificity, predictive values, and accuracy of the CAT for depression
| CAT score |
Sensitivity |
Specificity |
Positive Predictive Value |
Negative Predictive Value |
Accuracy |
| ≥10 |
100.00 |
29.87 |
15.63 |
100.00 |
37.93 |
| ≥20 |
70.00 |
78.16 |
26.92 |
95.77 |
77.32 |
| ≥30 |
30.00 |
96.55 |
50.00 |
92.31 |
89.69 |
Download Excel Table
Discussion
COPD is associated with multiple comorbidities [3, 19]. In individuals with COPD, depression is significantly associated with decreased functional status, impaired quality of life, disease progression, and mortality [9]. It is important to focus on early screening and management of depression [20, 21]. However, depression in COPD patients is under-recognized and often undiagnosed since the symptoms are not disease-specific [20]. Without objective evidence such as that obtained by screening tools, it is difficult to refer patients to a psychiatrist, even if depression is considered during routine outpatient practice. Consequently, we aimed to investigate the relationship between the widely used CAT and depression as measured by the PHQ-9.
The main finding of the present study is that the PHQ-9 score was significantly higher in COPD patients with higher CAT scores. The data suggest that the CAT can be used as a predictor of depression. Our findings also show that significant depression among the groups based on the 2011 GOLD guidelines was only observed in the Gold B and D classes. A previous study demonstrated that the FEV1 does not adequately reflect all systemic manifestations present in COPD patients [22], whereas the CAT is more closely correlated with depression [14]. These findings suggest that physicians should carefully consider depression, particularly in symptomatic patients. Additionally, the previous study demonstrated that the prevalence of significant depression in stable COPD patients ranged between 10% and 42% [5]; in our study, the prevalence was 10.3%. This discrepancy could be partly attributed to the fact that our patients had relatively high competence levels for inhaler use. The clinical characteristics of the study group might also influence the prevalence of depression.
There are certain limitations to the present study. First, we did not use other scales for depression screening, such as the Hospital Anxiety and Depression Scale (HADS), the Center for Epidemiologic Studies-Depression (CES-D), or the Diagnostic and Statistical Manual of Mental Disorders-IV (DSM-IV), as the ‘gold standard’ [5]. Although the GOLD guidelines recommend that new COPD patients should have a detailed medical history, including an “assessment of feelings of depression”, there is no consensus on the most appropriate screening approach [1]. Second, we did not include other variables, such as the CAT items or comorbidities, in the multivariate analysis. Third, our sample size was relatively small.
In agreement with a previous study, significant depression is a common comorbidity that affects the health status of patients with COPD [19, 20]. Our study suggests that there is a correlation between the CAT and depression measured by the PHQ-9.
In conclusion, the CAT is a simple and valuable predictor of depression in COPD patients, and it should be frequently used to detect COPD patients with depression in clinical practice.
Acknowledgements
This study was supported by the research fund of Chungbuk National University Hospital in 2014.
REFERENCES
Rabe KF, Hurd S, Anzueto A, Barnes PJ, Buist SA, Calverley P, Fukuchi Y, Jenkins C, Rodriguez-Roisin R, van Weel C, Zielinski J. Global Initiative for Chronic Obstructive Lung Disease. Global strategy for the diagnosis, management, and prevention of chronic obstructive pulmonary disease: GOLD executive summary. Am J Respir Crit Care Med. 2007; 176 p. 532-555.

Halbert RJ, Natoli JL, Gano A, Badamgarav E, Buist AS, Mannino DM. Global burden of COPD: systematic review and meta-analysis. Eur Respir J. 2006; 28 p. 523-532.

Vanfleteren LE, Spruit MA, Groenen M, Gaffron S, van Empel VP, Bruijnzeel PL, Rutten EP, Op 't Roodt J, Wouters EF, Franssen FM. Clusters of comorbidities based on validated objective measurements and systemic inflammation in patients with chronic obstructive pulmonary disease. Am J Respir Crit Care Med. 2013; 187 p. 728-735.

Ng TP, Niti M, Tan WC, Cao Z, Ong KC, Eng P. Depressive symptoms and chronic obstructive pulmonary disease: effect on mortality, hospital readmission, symptom burden, functional status, and quality of life. Arch Intern Med. 2007; 167 p. 60-67.

Kunik ME, Roundy K, Veazeyk C, Souchek J, Richardson P, Wray NP, Stanley MA. Surprisingly high prevalence of anxiety and depression in chronic breathing disorders. Chest. 2005; 127 p. 1205-1211.

Norwood R. Prevalence and impact of depression in chronic obstructive pulmonary disease patients. Curr Opin Pulm Med. 2006; 12 p. 113-117.

Cully JA, Graham DP, Stanley MA, Ferguson CJ, Sharafkhaneh A, Souchek J, Kunik ME. Quality of life in patients with chronic obstructive pulmonary disease and comorbid anxiety or depression. Psychosomatics. 2006; 47 p. 312-319.

Gudmundsson G, Gislason T, Janson C, Lindberg E, Suppli Ulrik C, Brøndum E, Nieminen MM, Aine T, Hallin R, Bakke P. Depression, anxiety and health status after hospitalization for COPD: a multicentre study in the Nordic countries. Respir Med. 2006; 100 p. 87-93.

Negi H, Sarkar M, Raval AD, Pandey K, Das P. Presence of depression & its risk factors in patients with chronic obstructive pulmonary disease. Indian J Med Res. 2014; 139 p. 402-408.

Kim HF, Kunik ME, Molinari VA, Hillman SL, Lalani S, Orengo CA, Petersen NJ, Nahas Z, Goodnight-White S. Functional impairment in COPD patients: the impact of anxiety and depression. Psychosomatics. 2000; 41 p. 465-471.

Jennings JH, Digiovine B, Obeid D, Frank C. The association between depressive symptoms and acute exacerbations of COPD. Lung. 2009; 187 p. 128-135.

Jones PW, Harding G, Berry P, Wiklund I, Chen WH, Kline Leidy N. Development and first validation of the COPD Assessment Test. Eur Respir J. 2009; 34 p. 648-654.

Mackay AJ, Donaldson GC, Patel AR, Jones PW, Hurst JR, Wedzicha JA. Usefulness of the Chronic Obstructive Pulmonary Disease Assessment Test to evaluate severity of COPD exacerbations. Am J Respir Crit Care Med. 2012; 185 p. 1218-1224.

Ghobadi H, Ahari SS, Kameli A, Lari SM. The Relationship between COPD Assessment Test (CAT) Scores and Severity of Airflow Obstruction in Stable COPD Patients. Tanaffos. 2012; 11 p. 22-26.

Lee S, Lee JS, Song JW, Choi CM, Shim TS, Kim TB, Cho YS, Moon HB, Lee SD, Oh YM. Validation of the Korean version of chronic obstructive pulmonary disease assessment test (CAT) and dyspnea-12 question-naire. Tuberc Respir Dis. 2010; 69 p. 171-176.

Han C, Jo SA, Kwak JH, Pae CU, Steffens D, Jo I, Park MH. Validation of the Patient Health Questionnaire-9 Korean version in the elderly population: the Ansan Geriatric Study. Compr Psychiatry. 2008; 49 p. 218-223.

Huang FY, Chung H, Kroenke K, Delucchi KL, Spitzer RL. Using the Patient Health Questionnaire-9 to measure depression among racially and ethnically diverse primary care patients. J Gen Intern Med. 2006; 21 p. 547-552.

Kroenke K, Spitzer RL, Williams JB. The PHQ-9: validity of a brief depression severity measure. J Gen In tern Med. 2001; 16 p. 606-613.

Miyazaki M, Nakamura H, Chubachi S, Sasaki M, Haraguchi M, Yoshida S, Tsuduki K, Shirahata T, Takahashi S, Minematsu N, Koh H, Nakamura M, Sakamaki F, Terashima T, Sayama K, Jones PW, Asano K, Betsuyaku T. Keio COPD Comorbidity Research (K-CCR) Group. Analysis of comorbid factors that increase the COPD assessment test scores. Respir Res. 2014; 15 p. 13-20.

Van Manen JG, Bindels PJ, Dekker FW, IJzermans CJ, van der Zee JS, Schadé E. Risk of depression in patients with chronic obstructive pulmonary disease and its determinants. Thorax. 2002; 57 p. 412-416.

Von Leupoldt A, Taube K, Lehmann K, Fritzsche A, Magnussen H. The impact of anxiety and depression on outcomes of pulmonary rehabilitation in patients with COPD. Chest. 2011; 140 p. 730-736.

Celli BR, Cote CG, Marin JM, Casanova C, Montes de Oca M, Mendez RA, Pinto Plata V, Cabral HJ. The body-mass index, airflow obstruction, dyspnea, and exercise capacity index in chronic obstructive pulmonary disease. N Engl J Med. 2004; 350 p. 1005-1012.